Sinusitis in Children
Overview
Sinusitis is an infection of the sinuses. These infections often happen after a cold or with allergies. There are 3 types of sinusitis:
- Short-term (acute). Symptoms of this type of infection last less than 12 weeks and get better with the correct treatment.
- Long-term (chronic). These symptoms last longer than 12 weeks.
- Recurrent. This means the infection comes back again and again. It means 3 or more episodes of acute sinusitis in a year.
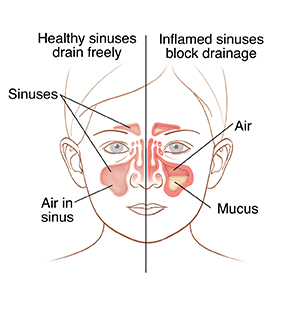
The sinuses are air-filled spaces (cavities) near the nose. They are lined with mucous membranes. There are 4 different sinuses:
- Ethmoid sinus. Located around the bridge of the nose. This sinus is present at birth and continues to grow.
- Maxillary sinus. Located around the cheeks. This sinus is also present at birth and continues to grow.
- Frontal sinus. Located in the area of the forehead. This sinus does not develop until around age 7.
- Sphenoid sinus. Located deep behind the nose. This sinus does not develop until the teen years.
Causes
When the sinuses are blocked with discharge, bacteria may start to grow. This leads to a sinus infection or sinusitis.
The most common bacteria that cause acute sinusitis include:
- Streptococcus pneumonia
- Haemophilus influenzae
- Moraxella catarrhalis
Symptoms
These are the most common symptoms of sinusitis:
- Stuffy nose
- Thick, colored drainage in the nose
- Drainage down the back of the throat (postnasal drip)
- Headache
- Cough
- Pain or soreness over sinuses
- Fever
- Loss of smell
The symptoms of sinusitis can seem like other health conditions. Make sure your child sees their healthcare provider for a diagnosis.
Risk Factors
A sinus infection sometimes happens after an upper respiratory infection or common cold. The cold causes swelling that can block the opening of the sinuses. This can cause a sinus infection. Allergies can also lead to sinusitis because of swelling and increased mucus. Other possible conditions that can lead to sinusitis include:
- Abnormal shape of the nose
- Infection from a tooth
- Nose injury
- Foreign object in the nose
- Birth defect with abnormality of the roof of the mouth (cleft palate)
- Problem with stomach acids (gastroesophageal reflux disease, or GERD)
- Cystic fibrosis and immunodeficiency syndromes
- Large adenoids (tissue behind the nose)
Immune problems or antibody deficiencies are risks for chronic sinus conditions.
Diagnosis
The healthcare provider will ask about your child’s symptoms and health history. They will give your child a physical exam. Your child may also have tests, such as:
- Sinus X-rays. An X-ray exam of the sinuses may help with the diagnosis.
- CT scan of the sinuses. A CT scan shows detailed images of any part of the body. They are more detailed than X-rays.
- Cultures from the sinuses. A swab of discharge from the nose may be taken. The sample is checked for bacteria or other germs.
Treatment
Treatment will depend on your child’s symptoms, age, and general health. It will also depend on how severe the condition is.
Acute sinusitis
Acute sinusitis may get better on its own. When it doesn’t, your child’s healthcare provider may prescribe:
- Antibiotics. If your child’s sinuses are infected with bacteria, antibiotics are given to kill the bacteria. If your child’s symptoms haven’t improved after 3 to 5 days, the provider may try a different antibiotic.
- Allergy medicines. For sinusitis caused by allergies, antihistamines and other allergy medicines can reduce swelling.
Don’t use over-the-counter decongestant nasal sprays without checking with your child’s healthcare provider. These sprays may make symptoms worse.
Recurrent sinusitis is also treated with antibiotic and allergy medicines. Your child’s provider may refer you to an ear, nose, and throat doctor (ENT or otolaryngologist) for testing and treatment.
Chronic sinusitis
Treatment for chronic sinusitis may include:
- ENT specialist visit. Your child may be referred to an ENT provider.
- Antibiotics. Your child may need to take antibiotics for a longer time. If bacteria aren’t the cause, antibiotics won’t help.
- Inhaled corticosteroid medicine. Nasal sprays or drops with steroids are often prescribed.
- Other medicines. Nasal sprays with antihistamines and decongestants, saline sprays or drops, or medicines to loosen and clear mucus may be prescribed.
- Allergy shots or immunotherapy. If your child has nasal allergies, shots may help reduce their reaction to allergens such as pollen, dust mites, or mold.
- Surgery. Surgery for chronic sinusitis is an option. But it is not done very often in children.
Care may also include:
- Fluids. A glass of water or juice every hour or two is a good rule. Fluids help thin mucus, allowing it to drain more easily. Fluids also help prevent dehydration.
- Saline wash. This helps keep the sinuses and nose moist. Ask your child’s healthcare provider or nurse for instructions.
- Warm compresses. Apply a warm, moist towel to your child’s nose, cheeks, and eyes to help ease pain in the face.
Complications
In very rare cases, acute sinusitis can result in a brain infection.
Prevention
There are things that can help your child prevent sinusitis. They include:
- Support a healthy lifestyle by providing a healthy diet, encouraging good fluid intake, and making time for physical exercise.
- Have your child use saline sprays, washes, or both. Use these often to keep the nose as moist as possible.
- Use a humidifier in dry indoor environments.
- Keep your child away from cigarette and cigar smoke. Don't allow smoking in your home or car.
- Keep your child away from things that cause allergy symptoms.
- Don't force water into the sinuses. For example, your child should not jump into water.
- Limit time in chlorinated pools. The chlorine can irritate the nose and sinuses.
- Teach your child when and how to wash their hands.
- Keep you and your child up-to-date on immunizations.
- Don't have close contact with people who have colds or other upper respiratory infections.
Key Points
- Sinusitis is an infection of the sinuses.
- When discharge from the nose is blocked, bacteria may start to grow. This leads to a sinus infection or sinusitis.
- Acute sinusitis may get better on its own. But if it doesn’t, medicine can be prescribed.
- For chronic sinusitis, the healthcare provider may refer your child to an ear, nose, and throat doctor (ENT) for testing and treatment.
- To help prevent sinusitis, encourage a healthy lifestyle and have your child use saline sprays or washes to keep the nose moist. Use a humidifier in dry inside areas.
Next Steps
Tips to help you get the most from a visit to your child’s healthcare provider:
- Know the reason for the visit and what you want to happen.
- Before your visit, write down questions you want answered.
- At the visit, write down the name of a new diagnosis and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you for your child.
- Know why a new medicine or treatment is prescribed and how it will help your child. Also know what the side effects are.
- Ask if your child’s condition can be treated in other ways.
- Know why a test or procedure is recommended and what the results could mean.
- Know what to expect if your child does not take the medicine or have the test or procedure.
- If your child has a follow-up appointment, write down the date, time, and purpose for that visit.
- Know how you can contact your child’s provider after office hours. This is important if your child becomes ill and you have questions or need advice.